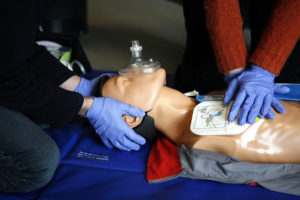
It’s a scenario we never want to picture ourselves in, coming upon someone in cardiac arrest (meaning the heart has essentially stopped beating). Whether formally trained or not, being the critical link between cardiac arrest and survival is a responsibility we all share.
An exhaustive study by the American Heart Association (AHA) showed that roughly 475,000 people in the United States alone die from cardiac arrest each year, with heart disease being the leading cause of cardiac arrest related death globally each year. More than 350,000 of these cardiac arrest deaths occur outside the hospital environment, meaning at home, at the gym, even at sporting events. The AHA states that nearly 90 percent of people who experience out-of-hospital cardiac arrest ultimately die, however that nearly 45 percent of cardiac arrest victims survived when early Cardiopulmonary Resuscitation (CPR) was administered. But what does this all mean?
What Is Cardiac Arrest?
People often confuse the term “heart attack” with “cardiac arrest,” but the two are not interchangeable. “Heart attack” refers to a state where the heart muscle is oxygen-deprived (for any number of reasons) but is still mechanically pumping, even if poorly. Cardiac arrest is when the heart has reached a state where it cannot beat properly (due to any number of reasons) and has essentially “arrested” or lost its ability to ineffectively pump.
When the heart stops pumping, oxygen-enriched blood stops circulating throughout the body and our vital organs, which depend on a steady oxygen supply to survive, begin to slowly die. This occurs faster in some organs than others, but the brain is unfortunately the most oxygen-demanding organ and is the first to experience cell death in the hypoxic (low-oxygen) environment. Brain damage has been found to occur four to six minutes after the cessation of blood flow, with irreversible brain cell death occurring after the six-minute mark.
According to a study published in 2017 by the American Medical Association, the average time from 9-1-1 call to Emergency Medical Services (EMS) arriving on-scene was seven minutes in the United States. This means that without CPR, by the time someone was found to be in cardiac arrest, 9-1-1 was called, and EMS arrived on scene, irreversible brain death would be almost guaranteed. CPR is the critical link in the chain of survival which was designed to artificially “pump” the heart and circulate blood until the heart’s normal pumping action was restored.
Resuscitation Guidelines for Cardiac Arrest
The AHA updates resuscitation guidelines typically every three to four years based on new data and statistics they find during the previous years’ studies; this means certain elements of CPR training are updated while some are removed when they’re found to negatively effect a person’s chance of survival. This is why it’s so important to keep your CPR training updated and consistent with your level of healthcare knowledge, so you are always practicing the most effective form of CPR which has been found to be most effective.
If you ever took a CPR class years ago, you might remember having to check for someone’s pulse to confirm its absence; this has been removed from the latest AHA layperson guidelines because in times of stress, it can be difficult to find someone’s carotid (the large artery along the side of the neck) pulse, and oftentimes people would feel their own pulse in their finger, rather than the victim’s pulse.
There are different recommendations for various levels of healthcare training, which means different steps and procedures to perform. In this article, we will cover bystander or layperson CPR recommendations, which are designed for people with little to no healthcare training.
The latest AHA guidelines as of 2017 (the last published revision) recommends when you find someone unresponsive (unable to be woken with a firm tap or shake), that you look, listen, and feel (with your hand resting on their chest) for signs of breathing. Agonal gasps (irregular, gasping, “guppy-like” breaths) are merely a reflex from an oxygen-deprived brain, and are not considered breathing. If no breathing (or agonal breathing) is noted, then it’s reasonable to assume the victim is in cardiac arrest and CPR must be initiated.
Calling 9-1-1
The first, and most crucial step to performing CPR is to activate the emergency response network: simply put, you must first call 9-1-1. This ensures paramedics can be dispatched and arrive quickly to take over and continue resuscitation with more advanced tools and techniques.
CPR alone cannot restore a heartbeat nor fix cardiac arrest—it is merely a life-prolonging measure meant to keep the person alive until advanced rescuers can arrive. Once 9-1-1 has been contacted, the dispatcher will likely provide instructions and ask questions over the phone to ensure CPR is being done properly.
How to Perform CPR
Once you have verified the person is unresponsive and not breathing, called 9-1-1, and given your location to emergency responders so they can respond, then you must begin immediate CPR with chest compressions. Again, in this article we are focusing on layperson CPR, which as of 2017 AHA guidelines, has become “Hands-Only CPR.”
Start by placing the person laying down on the floor or other hard surface (beds or couches are ineffective because of their cushioning and “springiness”). Kneel beside them, and locate the center of the chest; when we perform CPR, we want to be centered over the lower-half of the person’s sternum or “breastbone.” It’s the large flat bone in the center of the chest which connects both sides of the ribcage. Generally we will find this location at the nipple-line in the center of the chest. At this location, place one hand on the sternum, your other hand on top, and interlace your fingers. Position yourself so your upper-body is over their torso, and lock your elbows straight.
Begin compressing the chest straight down at a depth of roughly two inches or one-third the diameter of the chest. If it feels easy, you likely need to compress harder. We want to compress at a rate of 100-120 compressions per minute. If you don’t know how fast that is, compress to the tune of “Stayin’ Alive” by the Bee Gees, “Dancing Queen” by ABBA, or even “Sweet Home Alabama” by Lynyrd Skynyrd. Continue compressions until EMS arrives and tells you to stop or takes over for you.
Note it is no longer taught to administer rescue breaths via mouth-to-mouth for the layperson. If you have taken a CPR class and are trained to properly administer rescue breaths, then its reasonable to provide CPR in a 30:2 ratio, where you perform 30 compressions, followed by two rescue breaths, and repeat this process until EMS arrives.
When performing CPR properly, it’s very common to feel ribs cracking and breaking beneath your fingers. While this may be an uncomfortable sensation for the rescuer, it’s crucial that you DO NOT STOP giving compressions. Breaking ribs is a very common occurrence and despite the injury caused, a person can completely recover from broken ribs, but cannot recover from brain death.
Why Formal CPR Training Is Important
This article is not designed to replace a formal CPR class provided by a reputable institution, namely the AHA or Red Cross of America. It is highly recommended that you enroll in a proper CPR class where you can receive hands-on demonstration and instruction on how to effectively provide CPR by a licensed healthcare professional.
The purpose of this article is to demonstrate the importance of early CPR in out-of-hospital cardiac arrest and to display the importance of the bystander’s role in saving a person’s life. Statistically, four-out-of-five cardiac arrests occur at home; this means if called to perform CPR on someone, the life you would be saving would most likely be a family member. Although we never want to picture being placed in that situation, it’s important to prepare and equip ourselves with the knowledge necessary to save a life when we have the ability to. Providing effective CPR to a person in cardiac arrest will often double or even triple their chances of survival.
Enroll in a CPR class and keep your certification current so you can give your family and others the absolute best chance of survival in their time of need.
Photo: Rama/Wikimedia Commons